
The global concern of breast cancer continues to increase largely because of the aging and the growth of world population. Women treated for breast cancer or who have had mastectomies, lumpectomies, radiation treatment, lymph node removal, surgeries, infections, or trauma to the limbs often face a lifetime risk of developing lymphedema – a chronic condition that negatively affects the breast cancer survivors’ quality of life. One of the most unfortunate and dreaded outcomes of breast cancer treatment is Lymphedema.

What Is Lymphedema ?

Lymphedema is a chronic swelling of specific areas of the body due to the damage to the lymphatic system. Lymph fluid, which is a protein rich fluid, collects in the tissues when the lymph system is compromised. Protein in the tissues attracts additional water, thus resulting in chronic swelling. If left untreated, it may result in hardening of the skin tissue. If an effective treatment program is not initiated, the swelling may keep on increasing.
Most of the time, lymphedema develops in one arm or leg, but it can also be present in both arms and both legs. It may also occur in the hands or feet, and even in the chest, face, back, neck, genitals and abdomen.
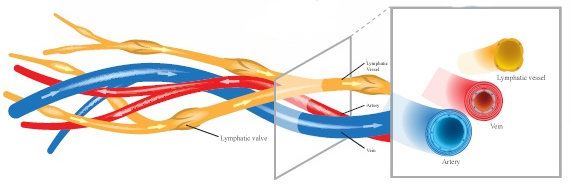
Types of Lymphedema
Primary Lymphedema
Primary lymphedema can occur due to any genetic mishap when the fetus is still in the uterus. Symptoms may be present at the time of birth or may develop later, often during puberty or pregnancy. It is most common in the legs, but may also occur in the arms and torso.
Secondary Lymphedema
Secondary lymphedema occurs as a result of damage to the lymphatic vessels usually traumatic injury. Secondary lymphedema occurs most commonly in the arms, but may also develop in the legs.
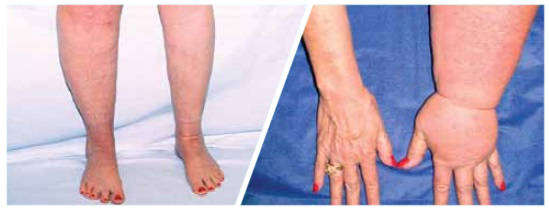
Lymphedema Symptoms
Breast cancer survivors with lymphedema often experience multiple symptoms such as swelling, heaviness, tightness, firmness, pain, soreness, tingling, stiffness, limb weakness, fatigue and impaired limb mobility of shoulder, arm, elbow, wrist, and fingers. These symptoms are the earliest signs of the increasing interstitial pressure changes that are associated with lymphedema.
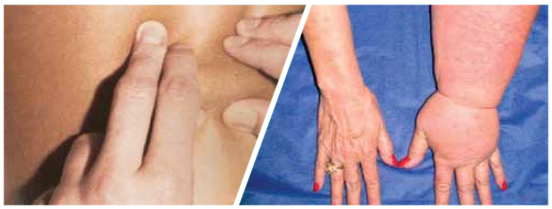
What To Do If Symptoms Occur?
Wearing custom lymphedema garments will provide external pressure to assist lymph drainage, thereby avoiding further swelling. Although swelling is sometimes reversible, in most cases, it is not and can lead to chronic lymphedema.
It is recommended to wear a lymphedema arm sleeve and lymphedema full leg garments if you engage in exercise, cleaning or any other outdoor task. If you don’t want the swelling to increase while flying, wear your compression garment. When the cabin pressure decreases, it puts stress on your lymphatic and circulatory systems, which can increase the swelling.
Diagnosing Breast Cancer Related Lymphedema
Breast cancer related lymphedema is a chronic syndrome of abnormal swelling of arms, legs and other body parts due to abnormal accumulation of protein rich lymph fluid in the interstitial tissue spaces. This accumulation occurs due to an imbalance between the production of lymph fluid and its transportation. Swelling is the main indication of lymhedema. Breast cancer related lymphedema can also occur in the shoulder, breast, and thoracic regions.
Management of Breast Cancer Related Lymphedema
There is no cure for breast cancer related lymphedema. Management of lymphedema will focus on swelling reduction and to maintain it by wearing compression garments such as lymphedema arm sleeve and full leg garments. Swelling reduction can be achieved by the skillful application of safe, reliable and non-invasive Complete Decongestive Therapy (CDT). This is proven to provide long term results for both primary and secondary lymphedema. CDT is performed by specially trained therapists, Certified Lymphatic Therapist. The treatment consists of four components: Manual Lymph Drainage (MLD), Graduated Compression Garments or bandages, Meticulous Skin Care, and Therapeutic Exercises.
Complete decongestive therapy (CDT) is the standard care for lymphedema but it is time-consuming, expensive, and requires lifelong maintenance. The therapy occurs in two phases:

Phase 1 – The lymph fluid is extracted out of the affected region and swelling is reduced using MLD techniques and bandaging. Ideally, this procedure is carried out daily or five days a week for 2-4 weeks depending upon the severity. Once the swelling is reduced, the patient is fitted with custom lymphedema garments.
Phase 2 – Fitting the patient with Lymphedema arm sleeve or Lymphedema full leg garments is the second phase. In this phase, the patient plays the major role in his or her ongoing self care. Wearing graduated compression garments, being meticulous about skin care, and performing self-manual lymph drainage and therapeutic exercises will assure continued success.
Closer Look at the Treatment
-
- Manual Lymph Drainage – Manual Lymphatic Drainage is a unique gentle type of skin massage necessary to promote lymph to drain out of a limb into an area that drains normally. This brings the affected part to normal size. Bandages are used in the Phase 1 and the compression garments are used in Phase 2.
-
- Skin Care – With lymphedema, the skin usually becomes dry and cracks easily, thus making it prone to infections. A low-pH lotion, free of alcohol and fragrances can be applied on the affected area to maintain the moisture of the skin and to protect it. If in case the infection develops, consult your physician immediately!
-
- Graduated Compression Garments – Graduated Custom Lymphedema garments are necessary to maintain the reduced limb and are designed to replace the bandages that were used earlier in the treatment. They are worn all throughout the day and a night garment should also be worn at night. The lymphedema arm sleeve helps to reduce swelling, improve circulation, and prevent the re-accumulation of the fluid in any body part. The garments must be worn every day.
- Exercise – A skilled therapist may recommend an exercise program in accordance with your needs and abilities. The exercise aids the muscular system to move lymph fluid out of the affected area. Moderate exercise such as swimming, walking, biking, light weight training and yoga are recommended.
Custom Lymphedema Garments – An Overview
As the name suggests, lymphedema arm sleeves and lymphedema full leg garments – apply pressure to the arm, hand, or trunk to help the lymph move in the right direction. As part of the overall treatment, custom lymphedema garments have proved to be the most effective of all in treating lymphedema.
All of the garments are made up of flexible fabric. Sleeves are tighter at the buttom than they are at the top. This helps to create a graded pressure that keeps the lymph moving out of the arm. There are available other variety of fabrics too that are softer, stiffer while others are made up of wool or latex.
In the case of mild lymphedema, lymphedema arm sleeves or lymphedema full leg garments can be the best suitable treatment. For stage 2 and stage 3 lymphedema, first Complete Decongestive Therapy is recommended in order to bring down the swelling. Thereafter, the patient is made to wear custom lymphedema garments to maintain those results and avoid further swelling. The lymphedema therapist will determine how often you need to wear it and for how long. You might also be asked to wear a different type of sleeve at night for more compression.
Tips For Buying And Managing Custom Lymphedema Garments
Tip #1 – Always buy your compression sleeves and garments from your certified lymphedema therapist or from a renowned medical company as recommended by your therapist.
Tip #2 – Have your sleeve or garment properly fitted by someone who has years of experience. An improperly fitted sleeve can make lymphedema worse as it might either apply too much or too little pressure on certain areas of the limb, thus making the situation worse.
Tip #3 – Consider buying two sleeves or garments so you can alternatively use them. Typically they need to be replaced every 3 to 6 months because they lose stretchiness over time.
Tip #4 – If you’re buying a compression sleeve, ask your lymphedema therapist whether you will be required to wear a glove or gauntlet on your hand too.
Tip #5 – Do not apply moisturizer on your arms, hands and legs prior putting on the sleeve. These beauty products can break down the elastic fibers in the sleeve over time.
Frequently Asked Questions
Does lymphedema ever go away?
If diagnosed early, lymphedema can be managed through proper treatment, quality compression garments, and good skin care. Management is the key to success.
Does my insurance plan cover compression garments?
Although insurance plans rarely cover the cost of compression sleeves and other garments ,you can check with your insurance company.
How do I care for my compression garments?
Daily wash and dry with mild detergent is recommended to maximize therapeutic effectiveness. Do not use fabric softeners, chlorine or bleach which may damage your garment.
Need Custom Lymphedema Garments and Arm Sleeves?
If you require custom fittings for lymphedema garments and compression sleeves, you have come to the right place! Pink Ribbon Boutique provides personalized, professional and discreet fittings for breast cancer survivors and anyone with lymphedema. We have a range of lymphedema arm sleeves and lymphedema full leg garments from major brands and our BOC certified fitters will work with you to get the best fit that helps you manage and control lymphedema. We also do alterations after you receive your custom lymphedema garments at absolutely no cost.
